How Weed Affects The Brain
We’re just starting to understand the complex mechanisms of cannabis and how they affect our brain. This includes everything from psychoactive effects to therapeutic benefits. What does research say about weed on the brain?
Is weed bad for your brain? What part of the brain does weed affect? If you’ve ever wondered how cannabis impacts the brain, you’re about to find out. In this article, we take a look at how cannabinoids influence our cognitive organ, from both sides of the debate. We’ll show you the potential benefits as well as possible dangers.
Contents:
How Cannabis Affects the Brain
Cannabis contains hundreds of different bioactive chemicals, including cannabinoids such as THC and CBD as well as terpenes and flavonoids. The human brain features 180 distinct regions[1], several different cell types (including 100 billion neurons), over 40 neurotransmitters, and countless receptors. As you can imagine, the relationship between this psychoactive plant and our biological computer is extremely complex. However, advances in botany, neuroscience, and physiology have allowed researchers to gain a solid, albeit early, understanding of how cannabis affects the brain.
A Primer on Brain Function
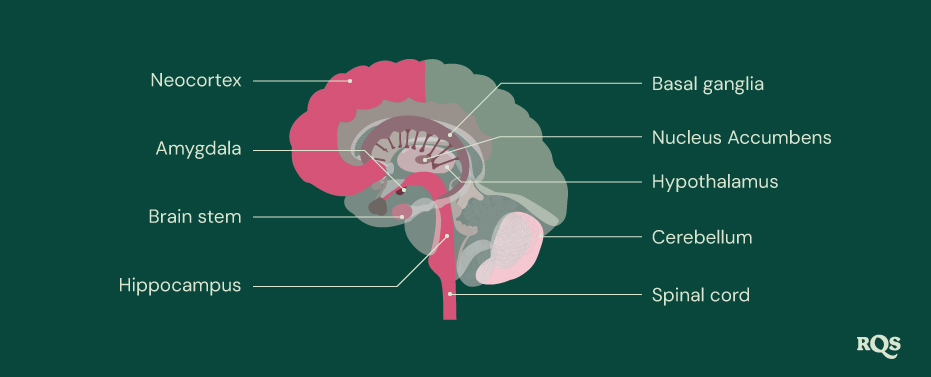
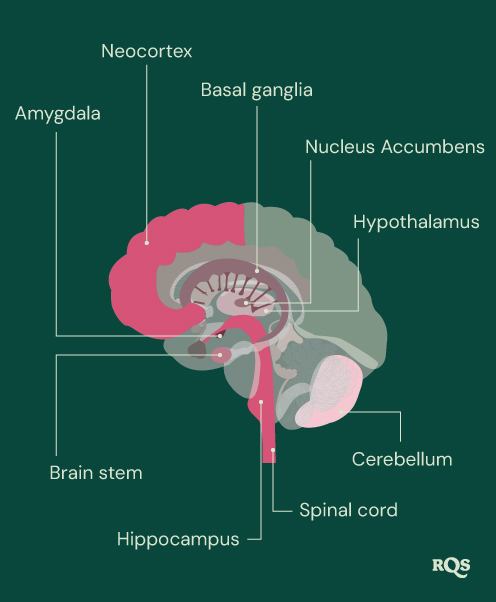
The brain holds the title of the most important organ in the human body (although we wouldn’t last very long without a heart or pair of lungs either). The reductionists among us might see the brain as nothing more than a lump of fat filled with electrical signals and capillaries. However, scientists have called the brain the most complex[2] thing we’ve discovered in the universe. Ultimately, the brain controls and regulates everything that happens in the human body, including:
- Thoughts and memory
- Emotion
- Touch, sight, hearing, taste, smell
- Breathing
- Temperature
An Introduction to the Endocannabinoid System
To understand how weed affects the brain, it’s important to become familiar with the endocannabinoid system (ECS). Known as the universal regulator of the human body, this large signalling network shows up everywhere from the central nervous system and digestive system to the skeleton and skin. The ECS helps to keep all of these systems running smoothly by keeping them within their “goldilocks zone”—a state of homeostasis. The ECS consists of three parts:
- Endocannabinoids: These signalling molecules are created on demand within cell membranes and bind to receptors on cell surfaces and within cells. The major endocannabinoids are anandamide and 2-AG.
- Cannabinoid receptors: These proteins are found on cell membranes and organelles (specialised structures within cells). Upon activation, they either spark or dampen chemical cascades within target cells.
- Enzymes: These proteins autumn into two categories: anabolic and catabolic. Anabolic enzymes make endocannabinoids from precursor molecules, whereas catabolic enzymes break them down after they’ve fulfiled their role.
In the brain, the ECS helps to maintain homeostasis by governing the flow of neurotransmitters. Unlike serotonin, dopamine, acetylcholine, and many other neurochemicals that travel in an antegrade fashion (from a presynaptic to a postsynaptic neuron), endocannabinoids can travel both ways. By going backward across the synaptic cleft, endocannabinoids are able to modulate the release of neurotransmitters from presynaptic neurons.
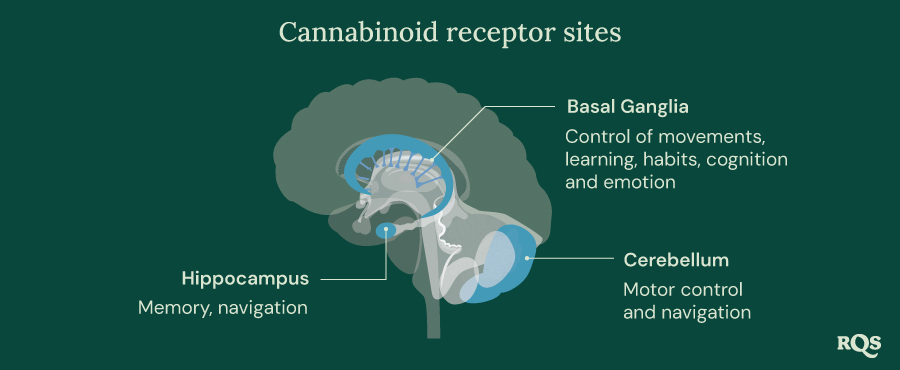
Pharmacodynamics: How Cannabinoids Move Through the Body
Cannabinoids such as THC and CBD produce their effects in several ways. They bind to cannabinoid receptors, serotonin receptors, and sites that make up the “expanded ECS”—a larger network known as the endocannabinoidome. However, how cannabinoids arrive at these receptors depends on how they are administered. The primary methods of consumption include:
- Inhalation: Smoking and vaping introduce cannabinoids into the lungs, where they diffuse into the bloodstream through small sacs called alveoli. From here, they are whisked toward the brain and pass through the blood–brain barrier. Once inside, they bind to cannabinoid receptors on the surface of neurons and other cell types found in the brain. Specifically, THC activates CB1 receptors, which is what causes us to feel high.
- Oral: Edible cannabis must first travel through the stomach and liver. This process converts THC into a metabolite called 11-hydroxy-THC. After processing, this molecule enters the systemic circulation and passes through the blood–brain barrier. This metabolite interacts with ECS receptors in a way that creates an even more potent psychoactive effect than THC.
- Sublingual: This method of consumption involves placing extracts and oils under the tongue. Cannabinoids diffuse into the capillary bed in the floor of the mouth and immediately enter the systemic circulation.
- Topical: Application of cannabinoids onto the skin activates ECS receptors found in our second-largest organ. Oils, lotions, creams, and balms only influence the ECS locally. Transdermal patches, however, deliver cannabinoids deeper and grant them access to the bloodstream.
Cannabis: Much More Than Just THC
As the principal psychoactive component of cannabis, THC gets a lot of attention. However, this molecule belongs to a large family of over 100 cannabis-derived cannabinoids. Moreover, this class of compounds exists alongside the hundreds of other bioactive secondary metabolites found in cannabis.
Among these, terpenes underpin the particular aroma and taste of each cultivar. These chemicals also interact with the ECS, and early research suggests that they might synergise with and amplify the effects of cannabinoids through a phenomenon known as the entourage effect.
The Potential Applications of Cannabis for the Brain
Ongoing studies are attempting to determine if cannabis produces a positive or detrimental effect on the human brain in terms of mood, cognitive function, and mental illness. Many of these research efforts focus on neurological symptoms and diseases. Check out what the current body of research says about the effects of cannabis on epilepsy, pain, ageing, and other conditions below. Note that this list is far from exhaustive!
1. Epilepsy
Epileptic seizures are caused by sudden bursts of electrical activity within the brain.
CBD has made headlines in the last decade as accounts of parents administering the cannabinoid to children with treatment-resistant epilepsy have come to the fore.
Larger-scale human trials have also set out to analyze the effects of CBD (specifically the cannabis-based medicine (Epidiolex) on children with rare forms of epilepsy such as Dravet syndrome and Lennox-Gastaut syndrome.
2. Concussion
As a form of traumatic brain injury, concussions occur following a bump or jolt to the head. They are common amongst athletes that participate in contact sports but can happen to anybody after a car accident or fall. Concussions vary in severity. Mild concussions involve no loss of consciousness and minor symptoms that fade within 15 minutes, whereas severe concussions cause a loss of consciousness and are potentially life-threatening.
Researchers are currently looking for ways to minimise the damage associated with concussions to protect the brain health of athletes and the general population. Early studies[3] are examining if cannabis use shortly after concussion may help to lower the symptom burden. Other findings suggest that the ECS modulates the pain response[4] following concussion.
3. Appetite
Many cannabis users are familiar with the munchies—a surge in appetite caused by THC. Cells in the hypothalamus are responsible for controlling appetite, and the ECS also plays a role in feeding behaviour[5]. While overeating can lead to several poor health outcomes, poor appetite occurs as a symptom of numerous conditions, and as a side effect of conventional cancer treatment and cancer distress. Researchers continue to test THC’s viability[6] as an appetite-stimulating agent in people with cancer and other health conditions affecting feeding behaviour.
4. Mood & Anxiety
Given its position throughout the limbic system, an area of the brain involved in behaviour and emotion, the ECS helps to regulate emotions, mood, and stress. With that in mind, studies are currently assessing the influence of CBD on anxiety in humans. Researchers have thus far tested the cannabinoid in cases of generalised social anxiety disorder[7], and have sought to determine if it alters blood flow[8] to areas of the brain involved in anxiety.
5. Pain
Persistent pain affects approximately 23% of the population[9] of the United Kingdom alone. Numerous conditions give rise to this state, including forms of arthritis, fibromyalgia, cancer, multiple sclerosis, and stomach ulcers. The ECS plays a significant role in pain signalling[10], and a host of ongoing studies[11] are pitting cannabis constituents against various models of pain.
6. Ageing
Age increases the risk of developing neurological diseases. Outside of these conditions, normal ageing also results in slower cognitive processing speed and a reduced ability to multitask. Research shows that the ECS plays an important role[12] in the progression of brain ageing, particularly in the hippocampus—the area of the brain responsible for learning and memory, which is vulnerable to neurodegeneration. Researchers are now testing the interaction[13] between cannabis and ageing in hopes of ascertaining both the potential positive and negative impact of its contents.
7. Alzheimer’s Disease
Is there a marijuana–Alzheimer’s link? Alzheimer’s disease impacts memory and cognitive function as proteins begin to build up around brain cells. Eventually, the disease destroys the brain to such a degree that it becomes fatal. Scientists are now assessing the possibility of utilising THC for Alzheimer’s disease. Thus far, studies[14] have begun to assess the cannabinoid’s potential to reduce buildup of beta-amyloid proteins.
8. Parkinson’s Disease
Researchers are also testing cannabinoids against different symptoms of Parkinson's disease, including motor symptoms[15]. Cannabinoids have spurred interest as potential therapeutic agents because the ECS occurs in the basal ganglia, a region of the brain responsible for motor control.
What Does Weed Actually Do to the Brain?
We’ve reviewed some of the cannabis plant’s potential for brain-related issues, but are the underlying mechanisms? Below, we take a closer look at the receptors and neurochemicals that cannabis constituents interact with.
Cannabinoid Receptors |
Cannabinoid receptors are a major part of the ECS. The two primary receptors of the system are CB1 and CB2. The CB1 receptor chiefly shows up in the brain and central nervous system. As mentioned, THC binds to this site as an agonist to produce the “high” associated with cannabis.
However, CB2 receptors are also expressed by certain cell types in the brain, and researchers are exploring this site as a potential target[16] for schizophrenia treatment. |
Anandamide and FAAH |
As well as targeting ECS receptors, cannabinoids also impact ECS enzymes. Early research shows that CBD inhibits an enzyme called FAAH. This protein breaks down the endocannabinoid anandamide—a molecule that plays an important role in mood and appetite. By inhibiting FAAH, CBD might temporarily elevate anandamide levels[17]. |
Serotonin |
Away from the ECS, several cannabinoids also activate serotonin receptors. Much like the ECS, the serotonergic system also comprises signalling molecules, receptors, and enzymes. Overall, this network helps to regulate sleep, appetite, and cognitive function. Both CBD and THC have an affinity for serotonin receptors[18], and therefore may have an ability to modulate mood. |
GABA and Glutamate |
GABA and glutamate are the yin and yang of neurotransmission. GABA works to inhibit neurological activity, whereas glutamate increases it. Excess levels of glutamate are implicated in obsessive-compulsive disorder, seizures, and anxiety. THC works to inhibit glutamate-releasing neurons[19], which can lead to a decreased sense of reward over time. What about CBD? This cannabinoid binds to GABA receptors. Researchers think this mechanism could show promise in the realm of seizures and anxiety. |
Dopamine |
Dopamine plays a crucial role in reward and motivation. It’s the reason getting high feels so good for a lot of people. THC causes a spike in dopamine when it binds to the CB1 receptor. As well as catalysing sensations of euphoria, this good feeling tells the brain to return to this behaviour again and again. |
Cannabinoid Receptors |
|
Cannabinoid receptors are a major part of the ECS. The two primary receptors of the system are CB1 and CB2. The CB1 receptor chiefly shows up in the brain and central nervous system. As mentioned, THC binds to this site as an agonist to produce the “high” associated with cannabis. However, CB2 receptors are also expressed by certain cell types in the brain, and researchers are exploring this site as a potential target[16] for schizophrenia treatment. |
Anandamide and FAAH |
| As well as targeting ECS receptors, cannabinoids also impact ECS enzymes. Early research shows that CBD inhibits an enzyme called FAAH. This protein breaks down the endocannabinoid anandamide—a molecule that plays an important role in mood and appetite. By inhibiting FAAH, CBD might temporarily elevate anandamide levels[17]. |
Serotonin |
| Away from the ECS, several cannabinoids also activate serotonin receptors. Much like the ECS, the serotonergic system also comprises signalling molecules, receptors, and enzymes. Overall, this network helps to regulate sleep, appetite, and cognitive function. Both CBD and THC have an affinity for serotonin receptors[18], and therefore may have an ability to modulate mood. |
GABA and Glutamate |
| GABA and glutamate are the yin and yang of neurotransmission. GABA works to inhibit neurological activity, whereas glutamate increases it. Excess levels of glutamate are implicated in obsessive-compulsive disorder, seizures, and anxiety. THC works to inhibit glutamate-releasing neurons[19], which can lead to a decreased sense of reward over time. What about CBD? This cannabinoid binds to GABA receptors. Researchers think this mechanism could show promise in the realm of seizures and anxiety. |
The Negative Effects of Cannabis on Brain Health
We know some of the possible benefits of weed for the brain, and their mechanisms, but what about the downsides? What follows are some of the plant’s potential detrimental effects.
Cannabis Use Disorder
Strong advocates of cannabis will tell you that cannabis isn’t addictive. However, around 30% of people who use cannabis develop cannabis use disorder[20] (CUD). The major signs of CUD include:
- Craving cannabis
- Failing to quit cannabis
- Continuing use despite deteriorating personal relationships
- Needing more cannabis to experience the same effects
CUD occurs because of how THC impacts the reward centre of the brain. The desirable sensations of being high motivate the brain to keep seeking out THC and repeating the same behaviour. However, the positive feeling associated with getting high gradually wanes as long-term THC exposure blunts dopamine levels and reduces CB1 receptor expression.
Psychosis and Schizophrenia
Cannabis and any potential links to psychosis and schizophrenia in at-risk populations are currently being studied. This ongoing investigation also includes any potential for THC to exacerbate symptoms in those already diagnosed. Neuroimaging studies[21] have also shown that THC exposure during adolescence can have a detrimental effect on brain morphology.
Memory Impairment
If you’ve ever smoked cannabis, you’ve probably experienced the short-term lapse in memory that often occurs while high. THC affects short-term memory by altering activity[22] in the hippocampus. Although only a minor annoyance for most people, short-term memory impairment can cause varying degrees of distress in sensitive individuals.
A Note on Responsible Cannabis Use
Not everyone experiences negative cognitive side effects from cannabis use. However, a small portion of users may face mental health challenges after heavy consumption. As a result, several organizations are working to encourage responsible cannabis use.
Royal Queen Seeds highlights the importance of mindful and moderate cannabis consumption, offering advice on how to use cannabis responsibly.
- Mapping the brain: scientists define 180 distinct regions, but what now? - Queensland Brain Institute - University of Queensland https://qbi.uq.edu.au
- Foreword - Discovering the Brain - NCBI Bookshelf https://www.ncbi.nlm.nih.gov
- Cannabis, alcohol and cigarette use during the acute post-concussion period - PubMed https://pubmed.ncbi.nlm.nih.gov
- Understanding the endocannabinoid system as a modulator of the trigeminal pain response to concussion - PMC https://www.ncbi.nlm.nih.gov
- Cannabinoid Receptor Signaling in Central Regulation of Feeding Behavior: A Mini-Review - PMC https://www.ncbi.nlm.nih.gov
- Efficacy of medicinal cannabis for appetite-related symptoms in people with cancer: A systematic review - PubMed https://pubmed.ncbi.nlm.nih.gov
- Cannabidiol Reduces the Anxiety Induced by Simulated Public Speaking in Treatment-Naïve Social Phobia Patients - PMC https://www.ncbi.nlm.nih.gov
- Effects of cannabidiol (CBD) on regional cerebral blood flow - PubMed https://pubmed.ncbi.nlm.nih.gov
- CKS is only available in the UK | NICE https://cks.nice.org.uk
- The role of the endocannabinoid system in pain - PubMed https://pubmed.ncbi.nlm.nih.gov
- Cannabis and Pain: A Clinical Review - PMC https://www.ncbi.nlm.nih.gov
- https://www.sciencedirect.com/science/article/abs/pii/S0047637415300099
- Interaction of Cannabis Use and Aging: From Molecule to Mind - PMC https://www.ncbi.nlm.nih.gov
- Cannabinoids remove plaque-forming Alzheimer’s proteins from brain cells - Salk Institute for Biological Studies https://www.salk.edu
- Pros and Cons of Marijuana in Treatment of Parkinson’s Disease - PMC https://www.ncbi.nlm.nih.gov
- Frontiers | Are CB2 Receptors a New Target for Schizophrenia Treatment? https://www.frontiersin.org
- Cannabidiol enhances anandamide signaling and alleviates psychotic symptoms of schizophrenia - PMC https://www.ncbi.nlm.nih.gov
- Cannabidiol modulates serotonergic transmission and reverses both allodynia and anxiety-like behavior in a model of neuropathic pain - PMC https://www.ncbi.nlm.nih.gov
- Why Marijuana Displeases | National Institute on Drug Abuse (NIDA) https://nida.nih.gov
- Addiction | Health Effects | Marijuana | CDC https://www.cdc.gov
- The Association Between Cannabis Use and Schizophrenia: Causative or Curative? A Systematic Review - PMC https://www.ncbi.nlm.nih.gov
- What are marijuana's long-term effects on the brain? | National Institute on Drug Abuse (NIDA) https://nida.nih.gov